
The most current map of intrathoracic lymph nodes is the International Association for the Study of Lung Cancer (IASLC) map. Stations 1–9 correspond to mediastinal nodal groups, while stations 10–14 represent hilar and other more peripheral extra mediastinal nodal groups. In contrast to the functional subdivisions, intrathoracic LN locations have been traditionally mapped into 14 stations according to their relationship to landmarks encountered during mediastinoscopy and thoracotomy for lung cancer. Dividing the mediastinum helps to narrow down the lengthy differential diagnoses, which can present in the thorax (including, but not limited to: infections like tuberculosis, the nodal spread of lung cancer, sarcoidosis, lymphoma, silicosis, and asbestosis). Lymph nodes (LNs) are present in all three functional compartments of the mediastinum, though most lymphatic tissue is found in the anterior and middle compartments, and the etiology of lymphatic pathology varies by subdivision. These subdivisions are used to describe the locations of lesions, thereby helping to facilitate differential diagnoses and communication between providers. The mediastinum is classically subdivided into three functional divisions: anterior (pre-vascular), middle (visceral), and posterior (paravertebral) mediastinum. The presence of necrotic/cystic areas is also highly predictive of metastatic disease compared to benign nodes in patients with head and neck cancer 5.The mediastinal compartment contains multiple critical organs and vessels and serves as the central hub for lymphatic drainage. Some studies compared the relative value of these different features, finding that minimal axial (short-axis) diameter was a better classifier for metastatic disease than maximal axial (long-axis) diameter or longest coronal (longitudinal) diameter 1,5. evidence of extranodal extension, including indistinct nodal margins, irregular nodal capsular enhancement, and infiltration into adjacent fat or muscle. 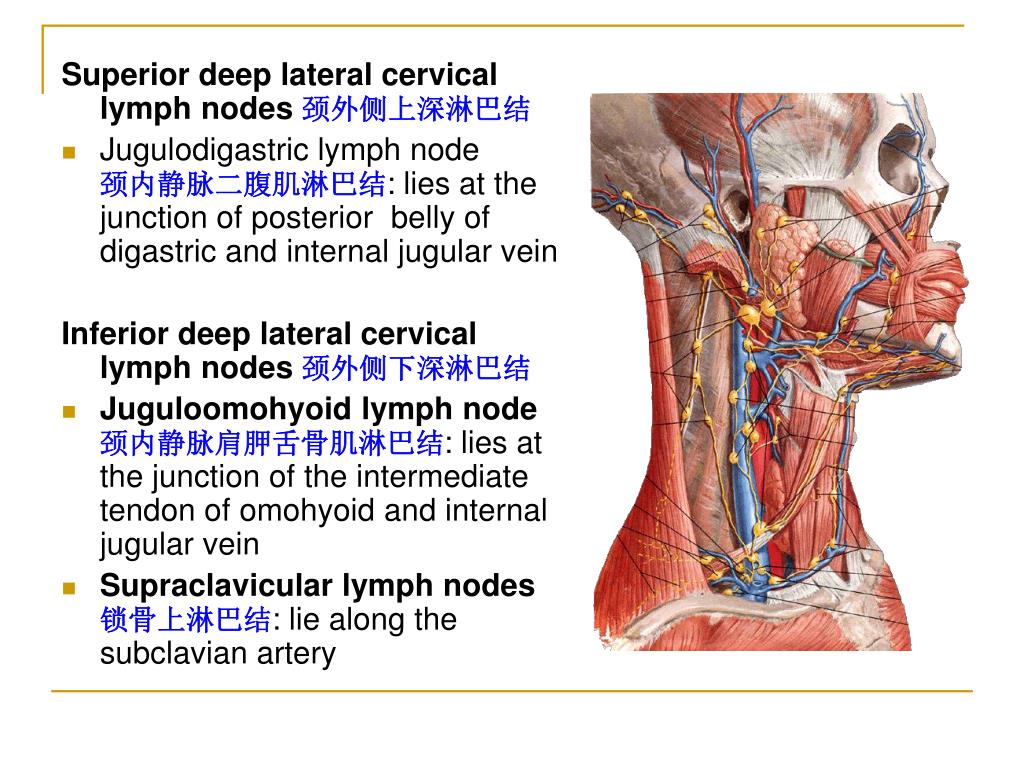
necrotic/cystic areas (low attenuation on CT, focal high T2 signal intensity on MR, hypoenhancing area with or without rim enhancement) 1,2.cluster of three or more borderline nodes (each ≥8 mm short-axis diameter, except >9 mm in the level II/subdigastric region) 1.maximize sensitivity (98%) and negative predictive value: ≥5 mm. 
maximize the sum of sensitivity and specificity: ≥12-15 mm.longest axial diameter cutoff criteria depend on which performance characteristic is of most interest (the following applies to level II and III nodes) 4:.any visible in the medial retropharyngeal group 2.≥5 mm in the lateral retropharyngeal group 2.≥11 mm in level II (subdigastric region) 1. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
